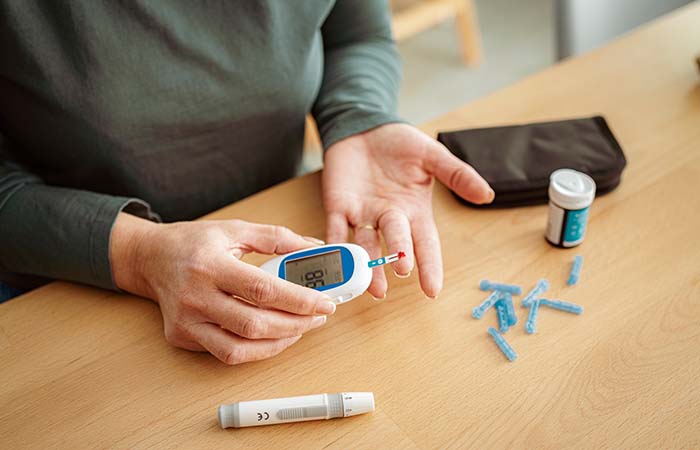
Diabetes management: Pharmacies on the frontline
In Population Health
Follow this topic
Bookmark
Record learning outcomes
You and your team are increasingly central to diabetes prevention, offering accessible risk assessment, early support, practical guidance and helping patients manage its impact. Sarah Clark reports
With diabetes prevalence continuing to rise, there is growing interest in whether community pharmacies could play a greater role in identifying people at risk earlier, potentially through a screening service similar to the hypertension case-finding programme. Earlier detection could help reduce pressure on NHS services by preventing serious and costly complications, in addition to the valuable support pharmacy teams currently offer customers living with diabetes or at risk of developing the condition.
Jackie Higgins, senior clinical advisor at Diabetes UK suggests that pharmacy teams already play a vital role by providing advice on reducing their risk, prevention and medicine management.
“The symptoms of type 2 diabetes may not be obvious, and with increasing numbers of people developing this life-changing condition, it’s vital that people know their risk,” says Higgins. “Through Diabetes UK’s partnership with Tesco, for example, pharmacy teams now provide specialist information and support for customers to help lower their risk of developing type 2.
“Customers can take a Diabetes UK risk assessment in-store at more than 350 Tesco pharmacies without an appointment. Specially trained staff can also advise people living with type 2 diabetes on aspects of managing the condition, including medication and as well as offering practical tips and support.”
Pharmacists based in designated locations listed on the NHS website can also refer patients at risk of type 2 diabetes to the Healthier You: NHS Diabetes Prevention Programme, if they meet eligibility criteria.
Early detection
Pharmacists play an increasing role in prevention and early detection, too. They can support people with all types of diabetes to manage their condition, helping people reduce their risk of diabetes-related complications. Diabetes UK encourages pharmacy staff to engage people with diabetes and ask them about their general health, advises Higgins, particularly if they are making enquiries about products which may be related to diabetes, such as foot care products and compression hosiery.
She comments: “Asking customers about their general health when they are ordering or collecting their diabetes medications is a good approach. Signposting to trusted sources containing further information would also be useful. The Diabetes UK website is a good starting point.”
Pharmacists can provide guidance on the importance of regular foot checks and offer education and advice on managing foot conditions. In addition, using tools such as ACT NOW, can equip pharmacists to be able to advise people about when they should see their doctor about a foot problem. Diabetes UK also encourages clinical pharmacists to carry out enhanced structured medication reviews.
The National Pharmacy Association (NPA) has highlighted new opportunities for pharmacies to expand their clinical services, including screening for cardiovascular risk and diabetes, as part of its response to the NHS 10-year plan, and in September 2024 the Company Chemists’ Association (CCA) called for a pharmacy diabetes screening service along the lines of the hypertension case-finding service, which the CCA claimed could save the NHS £50m a year by catching people with diabetes before serious complications develop.
Malcolm Harrison, chief executive of the CCA, suggests that as pharmacies have been identifying people at risk of cardiovascular disease through screening for elevated blood pressure since 2021, a similar pathway could be applied for a diabetes screening service. “This would mean that the service would be familiar to patients and pharmacy teams – and therefore quickly scalable. Patients could come to pharmacies and complete a questionnaire and take a finger prick blood test. Depending on their results, a pharmacist could either give advice, support them with lifestyle changes underpinned by follow-up point-of-care testing (PoCT), or refer them to their GP. In the future, we would expect any initiation of treatment to begin via a prescribing pharmacist.”
Pharmacy screening
He believes that PoCT can play a critical role in identifying those with diabetes or crucially those in a ‘pre-diabetic state’, and there are already examples of current success in this area. “Community pharmacies, renowned for their accessibility, combined with the ease of use of PoCT services, offer a new way to tackle this ever-growing health challenge. Community pharmacies have proven their ability to screen patients through programmes like the Blood Pressure Check Service and Pharmacy First.
“Later this year, all newly qualified pharmacists will be independent prescribers – as such, commissioners need to ensure there are services to prescribe against – a diabetes screening service could provide such an opportunity.”
Harrison emphasises that additional funding will be imperative to stabilise all pharmacies within the sector and ensure that the core supply function is maintained. “If pharmacies are commissioned to administer more services, this would need to be supported with appropriate, additional funding.”
It’s also worth noting that adequate training, restructuring of roles, and possible upskilling in PoCT are longstanding considerations that feature in the discourse around expansion of clinical services such as diabetes and hypertension screening in community pharmacy. Pharmacy staff will need to be offered appropriate training so that they are competent in both measurement and interpretation before pharmacies introduce this type.
The UK Clinical Pharmacy Association (UKCPA) has dedicated diabetes and endocrinology communities that offer education, networking, and training opportunities for pharmacists who are looking to expand their clinical roles, which may be a pathway towards building capability for diabetes screening services.
Gurpreet Kaur, diabetes medicines optimisation lead and Black Country integrated care board and UKCPA diabetes committee member, suggests that as diabetes prevalence continues to rise, community pharmacies could certainly play a greater role in earlier identification of people at risk, through offering screening services. “It could work in two ways, depending on funding - either opportunistically or via booked appointments as part of the future integrated neighbourhood health model of care,” she says. “Using standardised risk assessment tools can identify patients for additional blood tests, for example, Diabetes UK know your risk score and QDiabetes.”
Blood tests (random or fasting finger-prick blood glucose testing) are another suggestion, although Kaur suggests that HbA1c would be the ideal option.
“Although point-of- care devices are already available, local pathology services very often don’t approve them. Also, the communication of primary care results isn’t input into clinical systems, which leads to a need for repeat testing at GP practices. PoCT could be used for people assessed as being at risk, or high risk, as part of their initial screening through locally designed pathways, and support then given to patients who need a follow-up, if there’s a positive result that requires further investigation.”
For screening services to work effectively, though, data sharing needs to be in place with GP practices to make sure that any results and follow-ups are linked to a patient’s record – something the pharmacy sector is already advocating for.
Once diagnosed, people living with diabetes can turn to pharmacy teams for support with their condition, for example by helping patients to monitor their diabetes properly.
But there are pitfalls, and important considerations if patients are to be expected to take over monitoring such important aspects of their health. In the case of blood glucose monitoring, patients are regularly issued with new meters, says Kaur, which gives pharmacy staff the perfect opportunity to make sure they know how to use them, along with continuous glucose monitoring sensors like Freestyle Libre 2+ or Dexcom 1+.
“These get updated within the local health economy frequently,” says Kaur. “There’s an increasing emphasis on using apps to track blood glucose readings. All of these require support, but health literacy can be a challenge for some people. As pharmacies are generally more accessible, with appropriate funding they could support digital uptake locally and provide training/upskilling opportunities for pharmacy teams, as part of a wider healthcare neighbourhood team.”
Pharmacy staff are invaluable when it comes to ensuring medication adherence – especially through advising about the correct injectable therapy technique. They can also advise on the right storage and disposal of sharps and educate patients around things like sick day rules, which advise staying hydrated, frequent blood sugar/ketone monitoring, maintaining insulin, adequate carbohydrate intake and knowing when to contact a healthcare professional.
“Illness raises blood sugar levels and increases the risk of dehydration, especially if the patient is experiencing vomiting or fever,” advises Kaur. “Patients may visit a pharmacy for advice or support with minor ailment remedies, and this gives pharmacy teams the perfect opportunity to provide advice about using their medications during periods of sickness.”
With national issues surrounding medicines shortages and discontinuations, as well as the uptake of generic and biosimilar medication for cost-efficiencies, community pharmacy is very often involved in the supply chain – and pharmacists are likely to have to communicate any changes in therapies. This embeds the pharmacy team as key individuals to support medicines safety and reduce risk from harm from communication in changes that are made by prescribers.
Kaur suggests that as lifestyle and behaviour support such as weight management, smoking cessation, healthy eating and exercise advice and advertising of local services are already available in pharmacies, building in conversations about eye and foot health checks and even depression scores would be another avenue to explore to support people living with diabetes holistically in the community setting. “In addition, pharmacies need to be able to signpost local pathways for referral to suitable services – and make sure that any red flag escalations are appropriately managed,” she says. “The infrastructure for the sharing of notes and inputting of information to allow access to the wider team is still a gap – but it’s improving. This is very much an area for new prescribers in community pharmacies to consider.”