Testing, testing... for a healthier future
In Services Development
Follow this topic
Bookmark
Record learning outcomes

An estimated one in 15 people in the UK has diabetes and 300 million Europeans are living with hypertension, which is now seen as the prime contributing factor for global deaths. “While personal focus on exercise and eating well can contribute to a state of improvement, taking advantage of technological development to integrate a better state of health and wellness into the daily lives of customers is important,” says Charlie Fox, general manager at Omron Healthcare.
“By using the latest technology, pharmacists can improve care for customers. When pharmacists invest in upgraded technology, the customer is being given the opportunity to empower themselves to self-manage. For instance, there are now clinically validated home or on-the-go blood pressure monitors that provide the same accuracy of results as you would receive in your GP’s office.”
Long term plan for more screening
The NHS Long Term Plan outlines the important role of GP-based and community pharmacists in helping to reach more patients through screening, diagnostic and monitoring services. It promises to save 500,000 lives through preventive measures to tackle the major conditions that threaten our health. The plan will focus on prevention and early detection to stop an estimated 85,000 premature deaths a year.
“The NHS Long Term Plan provides enormous opportunities for pharmacy teams in all sectors to do even more to embed prevention and public health interventions in their daily practice,” says Gul Root, national pharmacy lead at Public Health England (PHE). “Community pharmacies are often embedded in some of our most deprived communities and are well placed to make a real difference to outcomes locally. PHE will continue to advocate the role of pharmacy teams in prevention and delivering public health interventions.”
Pharmacists already play an important role in illness prevention through managing long-term conditions and health promotion. “The importance of health screening and diagnostics cannot be over-emphasised,” says Olutayo Arikawe, Alphega Pharmacy member and pharmacist at The Priory Community Pharmacy in Dudley. “One of the key focus areas of the Long Term Plan is better prevention and detection to ensure more people receive care in the community. Pharmacies are able to support the community to live and age well by focusing on the prevention agenda.”
Focus on self-care and knowledge of our own health is improving, along with developments in the use of technology and increased media activity around monitoring our own health. “Pharmacy becomes the ideal location to support and advise customers, while offering services and products to help monitor and maintain health,” says Numark service development pharmacist Lucy Morris.
Health screening in pharmacy has been around a while, but it’s still not in the mainstay due to differences in services commissioned locally. “In the future, diagnostic testing in community pharmacy is going to be increasingly important, providing it aligns with the outcomes in the GP contract,” says Sadik Al-Hassan, Well pharmacist.
There are several areas of health screening and diagnostics where pharmacies could get more involved. These include supporting patients with respiratory disease in the use of new smart inhalers, which allow them to monitor their condition wherever they are. The Plan pledges to double the funding for the NHS diabetes prevention programme over the next five years and it has a target of increasing the percentage of early-stage cancers diagnosed from 50 per cent to 75 per cent by 2028. This will be done by raising awareness of cancers and making it easier to access screening and diagnostics tests through primary care services – it aims to reach more people with the NHS Health Check. Where people with high-risk conditions such as heart disease are picked up, pharmacists will be supported to help treat and refer them.
Why pharmacy?
“With so many people going into local pharmacies each day, it provides the NHS with opportunities for carrying out quality assured work relating to early detection and education about prevention of diseases,” says Hemant Patel, North East London LPC secretary. “Patient confidence is already high in community pharmacies and can be improved.” At NEL they have focused on NHS Health Checks, AF and blood pressure checks as well as MURs. “We have ambitions for using micro-spirometry to support the case for community pharmacists finding patients at risk of COPD,” he says. “Going forward, there would be a plethora of blood, urine, saliva and stool tests that can either be self-administered or done under the supervision of pharmacy staff. The important aspect to consider is the collection, organisation and use of patient-generated health data. Patients and caregivers can now independently capture and share their health data electronically with clinicians and researchers more frequently and from any location.”
 Pharmacists are well trained and qualified to provide health screening; they are accessible and open long hours. “The services are not only dependent on the pharmacist providing them, but are supported by qualified staff, too,” says Ms Arikawe. “I believe this is a growth area for the future.”
Pharmacists are well trained and qualified to provide health screening; they are accessible and open long hours. “The services are not only dependent on the pharmacist providing them, but are supported by qualified staff, too,” says Ms Arikawe. “I believe this is a growth area for the future.”
The availability of self-test kits allows customers to review and monitor elements of their own health. “Using self-test kits should be done with appropriate and safe advice and support, which creates a good opportunity for pharmacy to support patients,” says Cathy Crossthwaite, marketing co-ordinator at Numark
Mr Al-Hassan says Well’s private mole screening service is popular, along with free blood pressure checks. “Health screening is a growth area, as local commissioners once again see the value of pharmacy in identifying conditions such as AF and high blood pressure. “With increased reliability of readings on upper-arm models of BP monitors, they tend to be favoured by patients over wrist models. BP monitors with an ability to detect irregular heartbeat are a must,” he says.
Regular self-monitoring helps patients understand their condition. “According to May Measurement Month, increased access to BP screening is potentially the most effective way to reduce hypertension’s toll on health,” says Mr Fox. “By embracing innovative technology and providing access to diagnostic devices, pharmacists are helping customers minimise the impact monitoring has on their lives.”
Pharmacists have an important role to play in early diagnosis by talking to patients and encouraging them to see their doctor about unusual or persistent changes. “A community pharmacy team can have discussions about cervical, breast and bowel cancer screening and encourage eligible patients to register with a GP to make sure they receive an invitation,” says Weilin Wu, health information officer at Cancer Research UK.
According to Diabetes UK, less than half of those eligible for an NHS Health Check have received one in the past five years. The charity says there are 12.3 million people with a higher risk of developing type 2 diabetes who could reduce their risk by getting checked.
Pharmacist Ade Williams of Bedminster Pharmacy, Bristol, is pharmacy ambassador for Pancreatic Cancer Action. He believes that pharmacies are ideally placed to offer NHS Checks alongside GP surgeries to facilitate early cancer detection. “We know that early detection of pancreatic cancer not only improves survival, but also health outcome,” he says. “We can help to educate the public on signs to be aware of and those which should never be ignored. We can encourage customers to attend referral appointments and explain why it’s so important to diagnose cancer early. We know why patients don’t present early enough and pharmacists can help address this. A collaborative approach would mean more patients getting the checks.”
Helen Mee, head of health promotion and education at Bowel Cancer UK, says pharmacists are in a unique position to engage with high-risk, marginalised population groups. “Through their regular contact with these groups, pharmacists can play a vital role in increasing bowel cancer survival rates by raising awareness of screening and the benefits,” she says. “Nearly everyone survives bowel cancer if diagnosed at the earliest stage, but this drops significantly as the disease develops.” To help reach more patients at an earlier stage, she says pharmacies can provide leaflets and display posters and ensure all staff are trained so they have a better understanding of red-flag signs for bowel cancer.
Better overall patient care
Health screening and diagnostic services give pharmacies the opportunity to improve the patient care they offer. “In my pharmacy, improving technology for blood pressure checks, thanks to the addition of the Alphega Pharmacy vascular age check service, has helped us provide more health checks,” says Ms Arikawe. “Patients like the idea of finding their vascular age and being able to reduce health risks with lifestyle changes. The lung age test has helped us to direct customers to our smoking cessation clinic. These improvements are all opportunities to ensure greater use of the pharmacist and their team’s expertise.”
If you offer a screening or diagnostic service, it is important to have a quality assurance process in place to ensure reliability and accuracy. “With continual developments in technology, accuracy of results continues to improve,” says Ms Morris. “Using new technology to support your service may offer a USP and enable you to provide better patient care.”
In addition to devices, it is important to develop an understanding of data-driven health interventions. “The devices are only providing access to data which are going to be important in helping patients and health systems to improve outcomes,” says Mr Patel. “The focus is changing from treating each episode of illness in each individual to population health and using data linkage to get a better understanding of risks and service use patterns and predicting events and taking steps to nullify or reduce health risks. Patient-generated health data provides new opportunities to supply devices and help patients manage their health using their data.”
Next steps for innovation
Omron’s Evolv BP monitor can sync blood pressure readings to an Omron connect app, which allows users to track results and monitor progress. It can now link with Amazon's Alexa so users can find out the state of their heart health using a simple question.
Later this year, Omron’s HeartGuide, the first clinically validated wearable blood pressure monitor in the form of wristwatch, will be available in Europe. The device uses oscillometric technology and has an inflatable cuff within the watch band that takes the BP reading. The device also works like a smartwatch to give users a comprehensive picture of their heart health. A management app called HeartAdvisor will be launched at the same time.
The BioSure HIV self-test kit is being sold in Boots and Superdrug stores. It is available to independents through Fortuna Healthcare. It allows customers to self-test at home using a finger prick blood sample and gives a result in 15 minutes.
Smart Peak Flow is the first medically certified asthma-monitoring device. It plugs into a smartphone so sufferers can monitor and manage their condition better. The small mouthpiece plugs into the headphone jack of any smartphone and, with the accompanying app, can predict a potential asthma attack by up to seven days. The patient simply blows into the mouthpiece three times so the app can record variable lung function over time. Via the app, patients receive reminders, educational information and motivation. They can also share peak expiratory flow data instantly with doctors.
Community pharmacy initiatives
NHS Health Check
“The NHS Health Check helps identify who is at risk from some of the biggest preventable causes of early death and ill health and what they can do to lower or manage this risk,” says Professor Jamie Waterall, national lead for the NHS Health Check programme. “Every council has a duty to provide checks for people aged 40 to 74 years and many have had success working with pharmacies to do so. We are working hard to support councils to deliver this world-leading prevention programme and, as part of this, we share best practice on how the check can be delivered through pharmacy settings, to improve uptake across the community.”
Early testing for atrial fibrillation
As part of the NHS England Test Beds programme, a six-month trial in 21 pharmacies in Waltham Forest looked at early testing for atrial fibrillation (AF) using a Kardia hand-held device from AliveCor, which can spot AF in just 30 seconds. Anyone with an abnormal result received a rapid referral to a one-stop AF clinic at Whipps Cross hospital. The process took just two to three weeks compared with the national average wait of 12 weeks.
Out of 672 patients screened, about 7 per cent were identified with AF. “Combining innovative screening for AF in community pharmacies for over-65s with a rapid-access clinic offers a cost-effective strategy,” say independent evaluators of the pilot from University College London. “If replicated across England, an estimated 1,600 to 1,700 strokes would be prevented per year.”
“Professionals and patients not only got to experience the use of a novel piece of technology, but they experienced first hand the benefits and challenges of integrating a digital innovation into a clinical pathway,” says Hemant Patel, co-author author of the post-pilot study and North East London LPC secretary.
Sore throat test-and-treat service
This has been rolled out in pharmacies this year, with the aim of telling customers if they need antibiotics. It will reduce GP appointments and over-prescribing of antibiotics. After taking a throat swab, it takes just five minutes to give a result and antibiotics can be prescribed by the pharmacist, if needed.
Cystitis test-and-treat service
Boots pharmacies in London, Sheffield and Cardiff are piloting a cystitis test-and-treat service to give women faster access to the right treatment. Healthy.io’s DIP UTI test combines the traditional dipstick test, a pop-up cup to collect a sample and an app, which turns a smartphone camera into a clinical-grade analyser to test quickly for infection. If infection is found, the customer has the option to purchase antibiotics. It is hoped the test will reduce over-prescribing of antibiotics.
Coeliac test pilot
Community pharmacies were involved in a pilot study by Coeliac UK to help identify undiagnosed coeliac patients. Some 15 pharmacies were involved in the pilot, which offered a free test to customers presenting with signs of irritable bowel syndrom (IBS), diarrhoea or other gastro-intestinal problems. Almost 10 per cent of those tested had a positive result for coeliac disease.
Early cancer diagnosis
Lloydspharmacy has been involved in a cancer diagnosis project to improve early diagnosis rates. The multiple is supporting a partnership between the University of Manchester and Greater Manchester Cancer Vanguard Innovation. An online tool to check for cancer symptoms is being used by pharmacists at two Manchester stores. A questionnaire helps identify possible early signs. After completing it, patients are advised of their estimated risk and referred to their GP if necessary.
Category advice
- “Be proactive in promoting health screening devices. It’s also important not to assume you know what your customers would buy – develop conversations by explaining the options available,” says Olutayo Arikawe.
- “Try to ensure someone is on hand to answer any questions and support with use should a customer be looking to purchase a product. To go the extra mile for your customers, if they’re buying a BP monitor for example, offer to show them how to use it in the consultation room before they take it away,” says Lucy Morris.
- “There is a great opportunity to link health screening and diagnostics with your pharmacy’s healthy living campaign, enabling you to raise awareness by signposting patients to testing at the same time,” says Sadik Al Hassan.
Views from the P3pharmacy category panel |
||||||
|
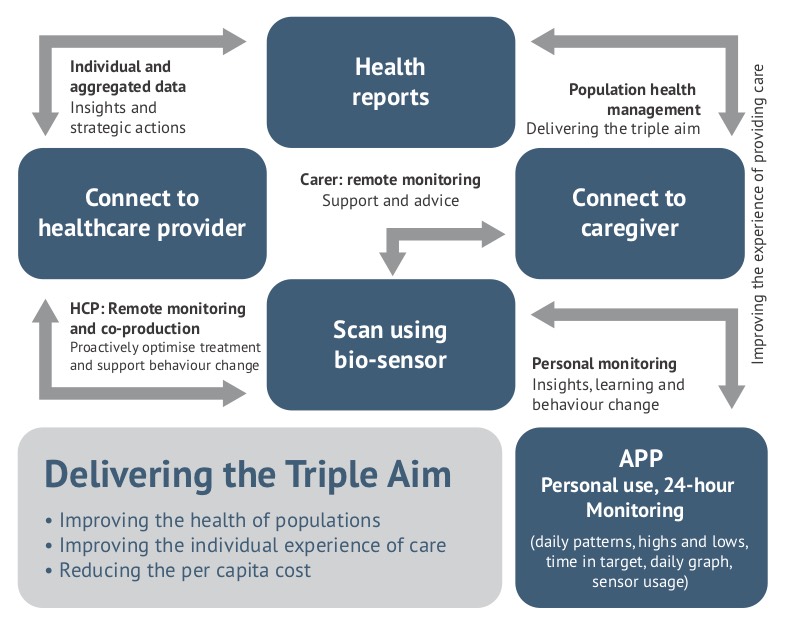
Patient-generated health data
Patient-generated health data (PGHD) are created, recorded, or gathered by or from patients (or family members or other caregivers) to help address a health concern, says Hemant Patel.
The relationship between patients and carers, and healthcare professionals and the health system is about to undergo a fundamental change as data is digitised for sharing, for analysis of disease progression, for monitoring population trends, to gain a better understanding of the distribution and determinants of health-related states or events (including disease), and to apply this to the control of diseases and other health problems.
Devices will only be providing access to data which are going to be important in helping to improve outcomes. So, in addition to devices, it will be important to develop an understanding of data driven health interventions.
An example of the dataflows that will be used to improve care of a diabetic patient is shown below.